Curious where the leaks are in your revenue cycle?
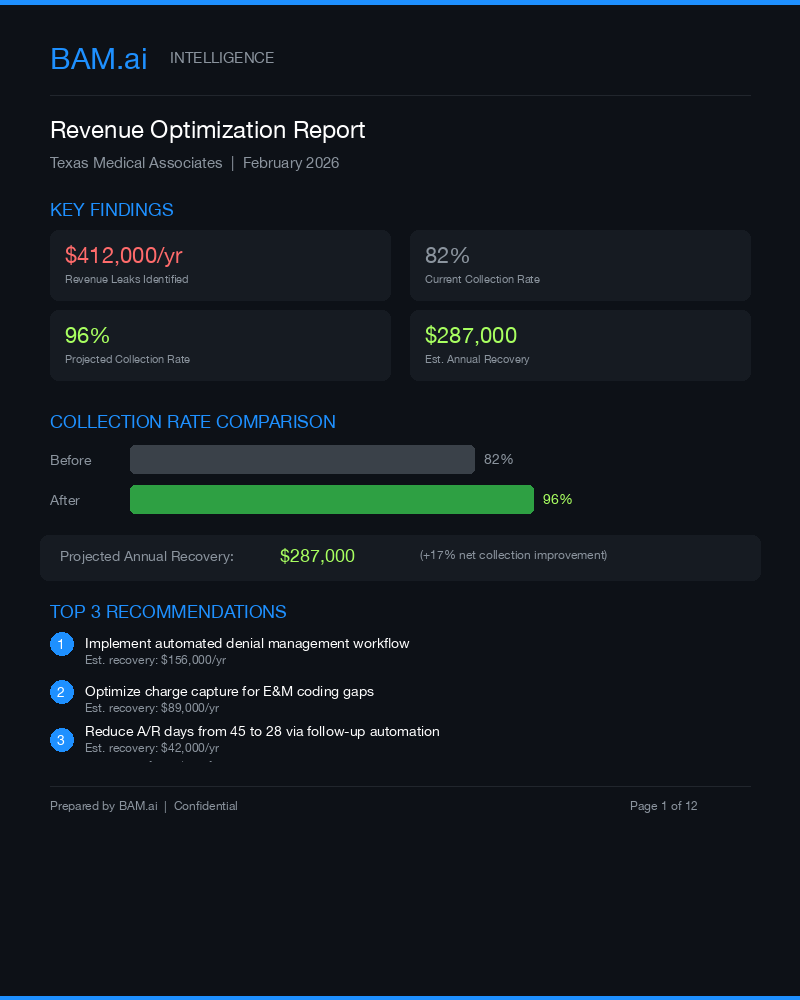
Take our Revenue Optimization Assessment and get a complimentary report showing exactly where you're losing money and how much you can recover.
- ✓ Identifies revenue leaks specific to your practice
- ✓ Custom ROI projection with dollar amounts
- ✓ Actionable recommendations you can use today
- ✓ Takes 5 minutes. No commitment.